Did you know that 1 in 23 men and 1 in 25 women have a lifetime risk of developing colorectal cancer? This form of cancer is the third most commonly diagnosed, and extensive research has been dedicated to understanding its causes, risk factors, early detection methods, and treatment options.
On a positive note, colorectal cancer (CRC) rates in adults over 50 have improved dramatically – incidence and death rates have fallen by more than 45% since the 1980s, thanks largely to better screening options and earlier detection.
And since March is Colorectal Cancer Awareness Month, it’s the perfect time to turn that progress into action by prioritizing your own screening and encouraging loved ones to do the same.
However, the news isn’t all good. In contrast, there has been an alarming rise in colorectal cancer cases and deaths among younger adults, particularly those aged 20-49. Some estimates suggest that colon cancer rates could increase by as much as 90% among individuals aged 20-34 by 2030.
So, what is behind this concerning trend? Research points to obesity as the most likely factor contributing to this uptick.
Table of Contents
What is Obesity in General?
Obesity is generally defined as an excessive amount of body fat. While the specific definition can vary across different medical systems and countries, a person is typically considered morbidly obese if their body mass index (BMI) exceeds 35. BMI is calculated by dividing an individual’s weight by their height squared, providing a fairly accurate measure of body fat percentage.
People with obesity are at higher risk for a range of diseases, including respiratory illnesses like COVID-19, high blood pressure, diabetes, sleep apnea, cardiovascular disease, and stroke, among others.
In light of this, researchers have increasingly focused on the link between obesity and cancer, and the results are troubling. Not only does obesity increase the likelihood of developing colorectal cancer, but it also hinders the effectiveness of prevention efforts, complicates treatment procedures, and worsens the overall prognosis.
All of these make early colonoscopy screening essential for people who are obese and who are 45 or younger.
Why is Colonoscopy Essential for Obese Patients?
Colonoscopy for obese patients is essential due to the increased risk of colorectal cancer (CRC), as excess body weight doubles the likelihood of developing adenomas (precancerous polyps) and contributes to 17% of cases. Obesity is also associated with higher mortality rates and more aggressive cancer, making early detection and polyp removal through screening essential.
Here are some major reasons for getting a colonoscopy done for obese people:
- Markedly Higher Risk: Obesity is closely linked to a higher incidence of colorectal cancer and related neoplasms.
- Preventive Measure: Colonoscopy helps identify and remove polyps before they progress to cancer, drastically lowering mortality rates.
- Lower Screening Participation: Despite the elevated risk, obese individuals tend to participate less in screenings, highlighting the need for proactive scheduling.
What are the Challenges of Colonoscopy in Obese Patients?
Colonoscopy in obese patients presents several challenges, including higher rates of inadequate bowel preparation, difficulty performing the procedure due to anatomical factors, and an increased risk of cardiopulmonary complications related to sedation. These challenges include extended cecal intubation times, greater scope looping, and a higher likelihood of missed lesions due to poor preparation.
Some of the main challenges of colonoscopy in obese patients are:
- Inadequate Bowel Preparation: Obesity is a significant predictor of poor bowel prep, often necessitating longer and more intensive preparation protocols to achieve a clear colon view.
- Technical Obstacles: Excess abdominal fat and a redundant colon complicate navigation, scope manipulation, and the application of manual pressure, resulting in prolonged and more difficult procedures.
- Sedation Risks: Obese individuals face a higher risk of complications from sedation due to comorbidities such as obstructive sleep apnea (OSA), cardiovascular conditions, and limited functional residual capacity, requiring enhanced anesthesia support.
- Reduced Detection Rates: Poor preparation and technical challenges can result in lower adenoma detection rates (ADR).
- Positioning Challenges: Standard lateral positioning may not suffice, often necessitating alternative positions, such as prone, to facilitate better navigation.
How Obesity Affects Colonoscopy Results?
The difficulties in conducting colonoscopies on obese patients are likely to increase as the obesity rate continues to rise. Recent studies in gastroenterology suggest that endoscopists should be prepared for a higher likelihood of incomplete procedures, longer procedure times, greater patient discomfort, and reduced tolerance when performing colonoscopy on obese individuals.
Additionally, research has shown that colorectal cancer (CRC) screening in obese patients tends to be less accurate, diminishing the positive outcomes typically seen with early detection screening.
Most concerning, however, is the emerging trend of physicians avoiding recommending colonoscopies for obese patients. This reluctance may stem from the increased risks associated with performing the procedure, competing healthcare priorities, staffing pressures, and potential bias or discrimination related to obesity.
Key Considerations and Guidelines for Obesity Colonoscopy Screening
Obese individuals are at an elevated risk for colorectal neoplasia, with guidelines typically recommending screening to begin at age 45, in line with the general population. However, for those with higher risk factors, screening may be advised earlier or more frequently. Proper, often split-dose, bowel preparation is crucial for obese patients due to their increased likelihood of inadequate cleansing and the potential for higher polyp detection rates.
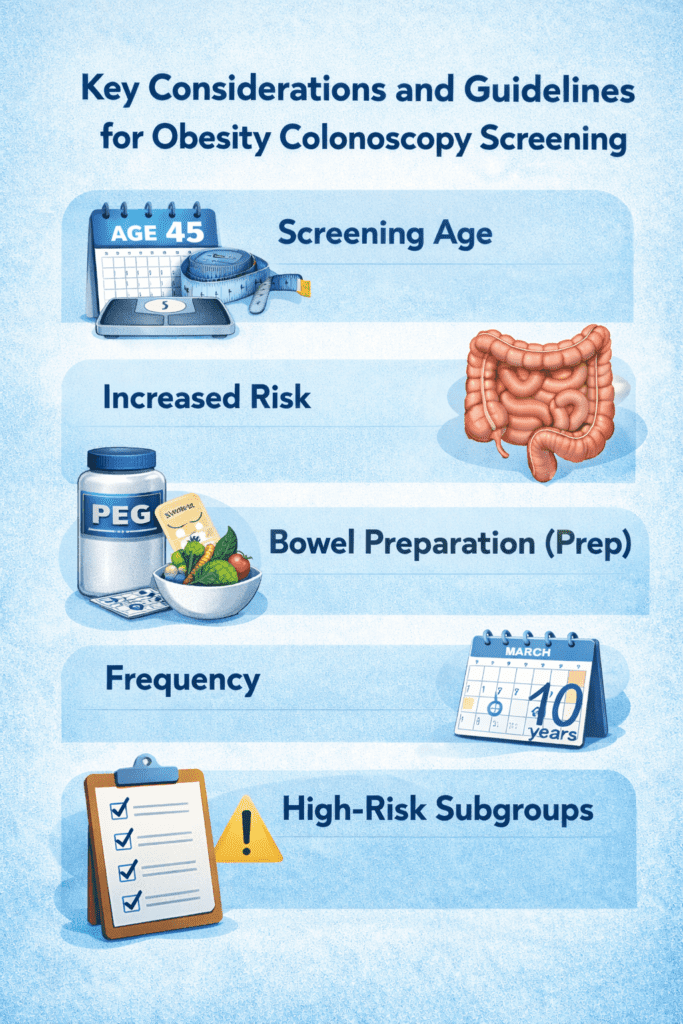
The important colonoscopy screening guidelines for obese people are:
- Screening Age: Begin colonoscopy screening at 45 for all average-risk adults, including those with obesity. Some studies suggest that men with obesity may benefit from starting screenings at age 40.
- Increased Risk: Obesity is associated with a higher incidence of colorectal neoplasia, including multiple adenomas or larger polyps.
- Bowel Preparation (Prep): Obese patients often require more robust bowel preparation, such as split-dose regimens, extended low-residue diets (up to 7 days), or higher-volume polyethylene glycol (PEG) solutions, to achieve adequate cleansing for clear visualization.
- Frequency: A 10-year interval between colonoscopies is typically recommended if initial results are normal.
- High-Risk Subgroups: Patients with additional risk factors may be considered at higher risk, making consistent adherence to screening guidelines essential.
What to Expect from a Colonoscopy if You are Obese?
Colonoscopy procedures for obese patients can present challenges, including more difficult bowel preparation, extended procedure times, and a higher risk of incomplete examination due to anatomical differences. Stronger prep protocols, alternative positioning (e.g., prone), and specialized sedation approaches may be necessary, along with an increased likelihood of requiring a follow-up examination.
Key Considerations for Obese Patients:
- Bowel Preparation: Obesity is a significant factor in poor bowel preparation, often necessitating more intensive or extended prep protocols to ensure adequate cleansing.
- Procedure Length & Difficulty: The procedure may take longer due to difficulties in passing the scope and navigating the colon.
- Positioning: You might be placed in alternative positions, such as prone (face-down), which has been shown to improve procedure success compared with the standard left-lateral position in obese patients.
- Sedation: Obese individuals face a greater risk of sedation-related complications, requiring more tailored sedation strategies, often managed by anesthesia professionals.
- Safety & Outcomes: Despite the increased technical challenges, the procedure remains essential. Techniques such as prone positioning, as highlighted in Gastrointestinal Endoscopy, can significantly improve both the speed and success rate of the procedure.
- Follow-up: Due to a higher risk of inadequate cleansing or missed lesions, a follow-up exam may be recommended sooner than for patients of average weight.
Be sure to discuss your weight and any related health conditions (e.g., sleep apnea, cardiovascular issues) with your gastroenterologist beforehand to ensure the team is fully prepared.
Learn more about the colonoscopy procedure here.
Why is Colonoscopy Important for Overweight Patients?
Colonoscopy is essential for overweight patients due to their higher risk of colorectal cancer and technical challenges during the procedure. Increased body fat can complicate bowel prep and the detection of polyps.
- Increased Procedure Difficulty: Overweight individuals often face more technical challenges during colonoscopy due to excess abdominal fat, making the procedure longer and more complex.
- Higher Risk of Incomplete Exam: Increased body mass may result in missed lesions or polyps, necessitating follow-up exams.
- Enhanced Bowel Preparation: Overweight patients often require more intensive bowel preparation protocols, such as split-dose regimens, to ensure adequate colon cleansing.
- Sedation Risks: Due to potential comorbidities, overweight patients may have a higher risk of sedation-related complications, necessitating careful management by anesthesia teams.
How Does Colonoscopy Screening Help Manage Obesity-Related Risks?
Obesity increases the risk of colorectal cancer, making colonoscopy screening crucial for early detection. The screening helps identify adenomas and allows for timely removal, reducing overall cancer mortality risk.
- Detecting Colorectal Cancer Early: Obesity increases the risk of colorectal cancer, making regular colonoscopy screening essential for early detection.
- Adenoma Detection: Obesity is linked to a higher prevalence of adenomas (precancerous polyps), which can be detected and removed during colonoscopy.
- Screening Frequency: Individuals with obesity may need more frequent colonoscopy screenings, starting at age 45, to manage their higher cancer risk.
- Customized Approach: Healthcare providers may suggest additional screenings or earlier start times depending on an individual’s obesity-related risks.
What Are the Challenges of Colonoscopy for High BMI Patients?
High BMI patients face more significant challenges during colonoscopy, including longer procedure times, difficult bowel preparation, and increased risk of incomplete exams. These factors necessitate a tailored screening approach.
- Difficult Navigation: High BMI patients may have more challenging colonoscopies due to excess body fat and a redundant colon, which makes it harder to maneuver the colonoscope.
- Prolonged Procedure Times: Colonoscopy in high BMI patients generally takes longer due to anatomical difficulties such as scope looping and longer cecal intubation times.
- More Intensive Prep: These patients often require more intensive bowel preparation, such as higher doses of PEG solutions or extended low-residue diets, to ensure the colon is adequately cleansed.
- Alternative Positioning: To improve success rates, high BMI patients may need to be positioned prone (face-down) during the procedure, which has been shown to yield better results.
Why is Colonoscopy Screening Recommended at Age 45?
The American Cancer Society recommends colonoscopy screening starting at age 45 for individuals of average risk. Early screenings are critical for obese patients, who face a higher risk of colorectal cancer.
- Standard Screening Age: The ACS recommends that all adults, including those with obesity, begin screening at age 45, as early detection is key to improving colorectal cancer survival rates.
- Obesity as a Risk Factor: For obese individuals, the risks associated with colorectal cancer increase, making early screenings even more important.
- Increased Screening Frequency: While the typical recommendation is every 10 years for average-risk individuals, obese patients may require screenings more frequently depending on their health status.
- Customized Guidelines: For those with obesity, some guidelines suggest screening may need to begin earlier or more frequently to account for the increased risk factors associated with higher BMI.
Getting a Colonoscopy at GATGI
At Gastroenterology Associates of Tidewater (GATGI), your health is our top priority. Here’s why we are the best GI near you for your colonoscopy:
- Convenient Scheduling: Our Open Access program allows you to schedule your colonoscopy directly, without a prior consultation, making the process simple and efficient for eligible patients.
- Board-Certified Physicians: All of our physicians are board-certified gastroenterologists, ensuring that you receive care from the most qualified professionals in the field.
- State-of-the-Art Equipment: We use the latest medical technology to deliver the highest-quality care and ensure the most accurate results during your colonoscopy.
- Integrated Care Approach: Our team approach means you receive personalized care tailored to your specific needs, supported by experienced professionals dedicated to your well-being.
- Access to Advanced Clinical Research: Led by top gastroenterologists, we offer patients access to cutting-edge research and the latest gastroenterology treatment options, ensuring you receive the most advanced care available.
Explore our services and begin your journey to better digestive health today with GATGI!
What We Do Differently: Tailored Approaches for Obese Patients
At Gastroenterology Associates of Tidewater, we provide personalized colonoscopy care to address the unique needs of obese patients.
1. Bowel Preparation
We use a combination of split-dose regimens, low-residue diets, and tailored solutions to ensure effective bowel cleansing for obese patients.
- Split-Dose Regimens: This method requires patients to take half the laxative the night before and the other half 4-6 hours before the procedure for better bowel preparation.
- Extended Low-Residue Diet: A low-residue diet for 3-5 days before the procedure improves visualization by reducing stool residue.
- High-Volume or Tailored Solutions: High-volume Polyethylene Glycol (PEG) solutions or customized agents help improve bowel cleansing and manage constipation effectively.
2. Sedation and Anesthesia Management
Special sedation protocols, led by anesthesia professionals, ensure comfort and safety, especially for patients with higher sedation risks like obesity or OSA.
- Anesthesia-Led Care: For Class III obesity or patients with Obstructive Sleep Apnea (OSA), we prefer Monitored Anesthesia Care (MAC) using propofol for optimal sedation.
- Airway Precautions: High-flow nasal oxygen (HFNC) and capnography (continuous CO2 monitoring) ensure safe ventilation during the procedure.
- Medication Management: To reduce aspiration risk, we recommend holding daily GLP-1 agonists (e.g., liraglutide) on the procedure day and weekly agents (e.g., semaglutide) for 7 days before the procedure.
3. Technical and Procedural Adjustments
To address anatomical challenges, we use specialized positioning, devices, and scopes to ensure successful colonoscopies in obese patients.
- Positioning: Starting in the prone (face-down) position helps reduce abdominal pressure and can ease insertion, improving success.
- Abdominal Pressure Devices: Tools such as the ColoWrap minimize scope looping and aid smoother navigation through the colon.
- Specialized Scopes: Pediatric or variable-stiffness colonoscopes help navigate a redundant or tortuous colon, improving procedure accuracy and comfort.
- Water Exchange/Immersion: Using water instead of air to distend the colon facilitates smoother navigation and a clearer view during the procedure.
- Staffing & Timing: Obese patients are scheduled first to ensure availability of specialized equipment and reduce the risk of prolonged fasting.
Your Health, Our Priority – Schedule Your Colonoscopy at GATGI Today!
Booking a colonoscopy at Gastroenterology Associates of Tidewater (GATGI) ensures you receive care from experienced gastroenterology physicians near you, who specialize in providing high-quality, compassionate care. Our board-certified gastrologists in Virginia Beach are dedicated to your digestive health, offering state-of-the-art procedures and personalized care. Don’t wait, and schedule your colonoscopy today to stay proactive about your health.