Celiac disease is more than a reaction to gluten – it is a lifelong autoimmune condition that needs consistent care, guidance, and monitoring. With the right support, patients can reduce symptoms, protect their digestive health, and prevent long-term complications. This article explains the importance of long-term management of celiac disease, what patients should know about diagnosis and ongoing care, and how GI specialists at GATGI help create personalized treatment plans to support better health, nutrition, and quality of life.
Table of Contents
What is Celiac Disease?
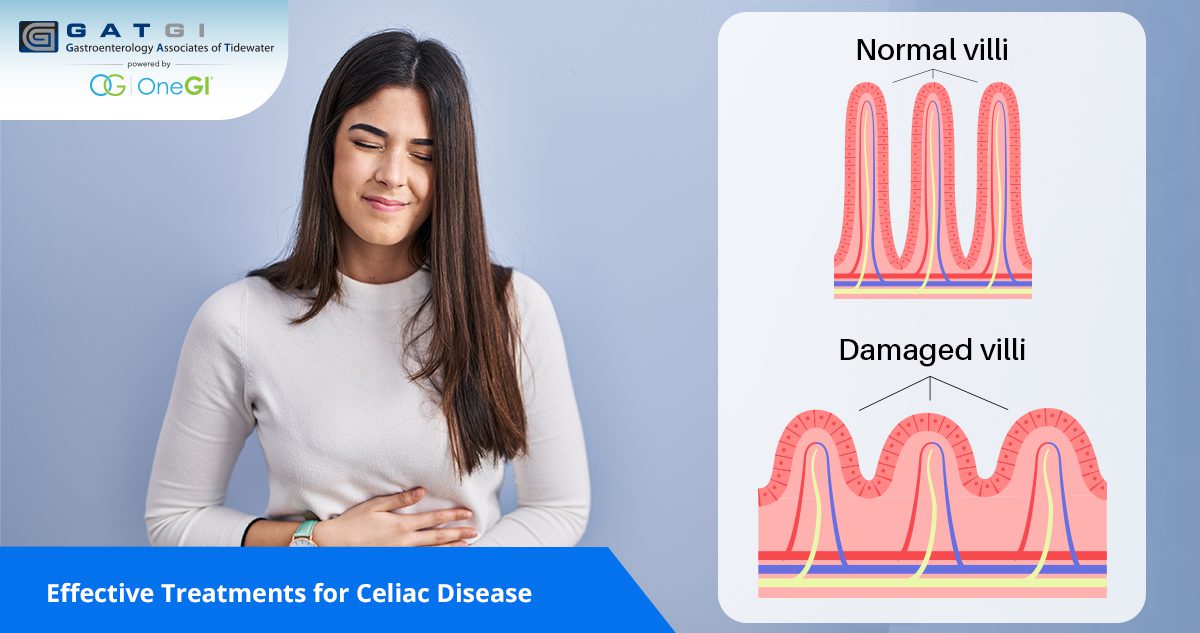
Celiac disease is a chronic autoimmune condition where eating gluten triggers the immune system to damage the small intestine. Gluten is a protein found in wheat, barley, and rye. Over time, this damage can make it harder for the body to absorb essential nutrients, leading to symptoms such as bloating, diarrhea, fatigue, weight changes, or anemia. Because symptoms can vary from person to person, proper diagnosis and long-term care from a GI specialist are important.
Why Does Celiac Disease Need Long-Term Management?
Celiac disease long-term management is essential because it is a lifelong autoimmune condition, not a short-term digestive issue. Even when symptoms improve, ongoing care helps protect the small intestine, prevent nutrient deficiencies, and reduce the risk of future complications.
- To monitor intestinal healing: The small intestine can take months or even years to heal after starting a gluten-free diet, so regular follow-ups help track progress.
- To detect hidden gluten exposure: Gluten can be found in sauces, processed foods, medications, or through cross-contact, sometimes causing damage without obvious symptoms.
- To check nutrient levels: Celiac disease can affect the absorption of iron, calcium, vitamin D, and other nutrients, increasing the risk of anemia, fatigue, and bone weakness.
- To prevent long-term complications: Untreated or poorly managed celiac disease may lead to osteoporosis, other autoimmune conditions, ongoing inflammation, or rare intestinal cancers.
- To support a balanced gluten-free lifestyle: GI specialists and dietitians help patients follow a safe, nutritious, and realistic long-term diet.
What Are the Common Symptoms of Celiac Disease?
Celiac disease symptoms can vary widely from person to person, and some people may have mild or “silent” symptoms. Because signs often overlap with other digestive conditions, proper testing by a GI expert is important.
- Bloating, gas, abdominal pain, or cramping
- Chronic diarrhea or constipation
- Fatigue, weakness, or unexplained weight changes
- Nausea, vomiting, or poor appetite
- Iron-deficiency anemia or nutrient deficiencies
- Skin rash, mouth ulcers, headaches, or joint pain
What Happens If Celiac Disease Is Untreated Long Term?
Untreated celiac disease can cause ongoing inflammation in the small intestine, making it harder for the body to absorb essential nutrients. Over time, this can affect digestive health, energy levels, bone strength, immunity, and overall well-being.
- Malnutrition and nutrient deficiencies: Long-term intestinal damage can lead to deficiencies in iron, vitamin D, calcium, and other nutrients.
- Anemia and fatigue: Poor nutrient absorption may cause ongoing tiredness, weakness, dizziness, or iron-deficiency anemia.
- Bone health problems: Untreated celiac disease may increase the risk of osteopenia, osteoporosis, and fractures.
- Reproductive and growth concerns: Some patients may experience infertility, pregnancy complications, delayed growth, or delayed puberty in children.
- Higher risk of other conditions: Poorly managed celiac disease may raise the risk of other autoimmune diseases, nerve-related symptoms, liver issues, and rare intestinal cancers.
- Long-term gut damage: Continued gluten exposure can prevent healing and may lead to more serious digestive complications.
Can Celiac Disease Be Cured or Only Managed?
Celiac disease cannot currently be cured, but with the right care, you can manage it well and live a healthy, comfortable life. The main treatment is a strict, lifelong gluten-free diet, which helps your small intestine heal and lowers the risk of complications. With regular follow-ups, nutritional guidance, and support from experienced experts, you can better control symptoms, avoid hidden gluten, and protect your long-term digestive health.
How to Manage Celiac Disease with the Right Medical Guidance?
Managing celiac disease starts with a strict, lifelong gluten-free diet, but you do not have to figure it out alone. The right medical guidance helps you avoid hidden gluten, restore nutrient levels, monitor healing, and prevent long-term digestive complications.
- Work with experienced GI experts: Your care team can confirm the diagnosis, track your symptoms, monitor intestinal healing, and address complications if they appear.
- Follow a personalized gluten-free diet: Avoid wheat, barley, and rye. Certified gluten-free oats may be safe for some people, but they should be introduced carefully with guidance.
- Get nutritional support: A dietitian or medical expert can help you build a balanced diet and check for common deficiencies, such as iron, vitamin D, calcium, and B12.
- Schedule regular follow-ups: After diagnosis, follow-up visits and blood tests help confirm that inflammation is improving and your body is responding well.
- Watch for hidden gluten: Gluten can be found in sauces, dressings, processed foods, medications, and cross-contact from shared kitchen surfaces.
- Monitor bone and overall health: Some patients may need bone density testing, vaccines, or additional screenings based on their health history.
- Ask for help if symptoms continue: Ongoing symptoms may mean hidden gluten exposure or, rarely, a more complex form of celiac disease that needs specialized care.
What Is Included in a Celiac Disease Treatment Plan?
A celiac disease treatment plan is designed to help your body heal, reduce symptoms, and prevent future complications. Since celiac disease is a lifelong condition, your plan usually includes diet changes, regular monitoring, and ongoing expert support.
1. Accurate Diagnosis and Testing
Proper testing may include blood work, antibody testing, genetic testing, and, in some cases, an endoscopy with biopsy to confirm intestinal damage.
2. A Strict Gluten-Free Diet
Avoiding wheat, barley, and rye is the main treatment. Even small amounts of gluten can trigger inflammation and delay healing.
3. Nutritional Support and Deficiency Monitoring
Experts may check your iron, calcium, vitamin D, B12, and folate levels to correct deficiencies and support overall health.
4. Follow-Up Visits and Symptom Tracking
Regular visits help monitor symptoms, review diet challenges, and ensure your body is responding well.
5. Screening for Long-Term Complications
Your care plan may include checks for bone health, anemia, autoimmune conditions, or ongoing intestinal inflammation.

Don’t Let Celiac Disease Hold You Back. Start Your Journey to Better Digestive Health Today.
Early intervention can help you manage symptoms and prevent long-term damage. If you're experiencing signs of celiac disease, our specialists are here to support you:
- Quick and Accurate Diagnosis: Get tested quickly and receive a clear understanding of your condition.
- Tailored Gluten-Free Plans: We'll guide you in creating a practical, lifelong diet plan tailored to your needs.
How GI Experts at GATGI Support Celiac Disease Long-Term Management
Managing celiac disease can feel overwhelming at first, but you do not have to manage every diet change, symptom, or follow-up alone. At GATGI, experienced GI experts provide effective gastrointestinal disease treatment, help you understand your condition, build a realistic care plan, and stay on track with long-term digestive health.
-
Personalized Care Plans Based on Your Symptoms and Health History
Your care plan is created around your diagnosis, symptoms, lifestyle, nutrition needs, and overall health history, so your treatment feels practical and personalized.
-
Ongoing Monitoring to Help Prevent Complications
Regular checkups, blood tests, and symptom reviews help track healing, identify nutrient deficiencies, and reduce the risk of long-term complications.
-
Guidance for Digestive Symptoms, Nutrition, and Lifestyle Adjustments
GATGI experts can help you manage bloating, discomfort, fatigue, and diet-related challenges while supporting a healthier gluten-free lifestyle.
-
Coordinated Care When Additional Support Is Needed
When needed, GATGI can coordinate care with dietitians or other providers to support your nutrition, bone health, and overall well-being.
When Should You See a GI Expert for Celiac Disease?
You should see a GI expert if you have ongoing digestive symptoms, unexplained fatigue, anemia, weight changes, or a family history of celiac disease. If you have already been diagnosed, regular visits are still important to monitor healing, check nutrient levels, and prevent complications. For patients searching for celiac disease doctors in Virginia Beach, GATGI provides expert support when symptoms continue despite a gluten-free diet or when long-term monitoring is needed.
Key Takeaways
- Celiac disease is a lifelong autoimmune condition that needs ongoing care.
- A strict gluten-free diet is the main way to manage symptoms and protect the small intestine.
- Regular follow-ups help monitor healing, nutrient levels, and possible complications.
- GATGI experts support patients with personalized long-term care and practical lifestyle guidance.
Get Long-Term Support for Celiac Disease with GATGI!
Managing celiac disease takes more than avoiding gluten. It takes ongoing guidance, regular monitoring, and a care plan that fits your life. With the right support, you can reduce symptoms, protect your digestive health, and feel more confident about daily food choices. If you are looking for celiac disease treatment in Virginia Beach, GATGI provides compassionate, expert care to help you manage your condition long term. Contact GATGI today to take the next step toward better digestive health.
Call 757-574-0798 to schedule an appointment!
Frequently Asked Questions
Can I develop celiac disease as an adult if I’ve eaten gluten my whole life?
Yes. Celiac disease can be triggered at any age, even if previous tests were negative (Village Emergency Centers, 2022). It often requires a genetic predisposition combined with a “triggering event” like surgery, viral infection, or severe stress.
Should my family members be tested even if they don’t have symptoms?
Because celiac disease is hereditary, first-degree relatives have a 1 in 10 risk of developing it (Cleveland Clinic, 2025). Screening is recommended for relatives because “silent” celiac disease can cause internal damage without obvious digestive issues.
How long does it take for symptoms to disappear after eating gluten by mistake?
While acute reactions typically peak within 24 hours, lingering symptoms like brain fog or joint pain can last up to 8 days. Complete intestinal healing takes much longer, often requiring months of a strict gluten-free diet (Celiac Disease Foundation, 2026).
Is a gluten-free diet enough, or do I need regular medical tests?
Diet alone isn’t always enough; regular blood tests and potential follow-up biopsies are necessary to ensure your antibody levels have normalized and your intestines are actually healing, as symptoms don’t always correlate with internal damage.