Ulcerative colitis is a chronic condition that affects your large intestine, causing inflammation and discomfort. If left untreated, it can impact your daily life. This article will guide you through understanding the symptoms, causes, and the best treatment options for managing ulcerative colitis, both medically and naturally.
By reading, you’ll learn to identify the early signs of ulcerative colitis and take control of your health, ensuring better disease management and an improved quality of life.
Table of Contents
What is Ulcerative Colitis?
Ulcerative colitis is a chronic disease of the large intestine, or colon, in which the lining of the colon becomes inflamed and develops tiny open sores or ulcers. This can cause discomfort and frequent emptying of the colon. By increasing awareness about this condition, we can potentially prevent its onset and effectively manage its impact.
Ulcerative colitis is one of the two types of Inflammatory Bowel Disease (IBD), the other being Crohn’s disease. Though both conditions share similar symptoms — abdominal pain, diarrhea, weight loss, and fatigue — they affect different parts of the gastrointestinal tract. Being aware of these similarities and differences is essential for understanding the disease and for facilitating early diagnosis.
The Importance of Early Detection in Ulcerative Colitis
Early detection of ulcerative colitis can greatly influence the management and progression of the disease. Detecting the disease in its initial stages allows for a more effective treatment strategy, potentially reducing flare-ups and promoting a better quality of life. Awareness of the symptoms and seeking prompt medical attention when they appear is key to early detection.
The early signs of ulcerative colitis are often subtle, but paying attention to symptoms like frequent diarrhea, abdominal discomfort, or blood in the stool can help identify the condition early. Early intervention may lead to a better prognosis and fewer complications.
What Are the First Symptoms of Ulcerative Colitis?
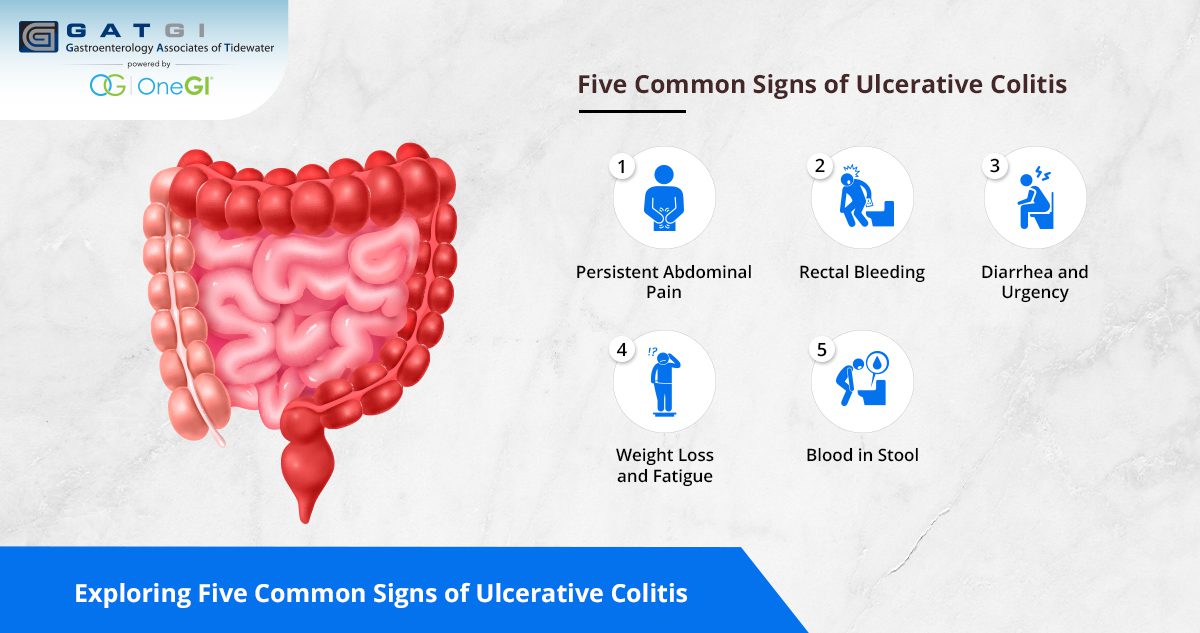
The first symptoms of ulcerative colitis typically involve gastrointestinal issues such as:
- Persistent diarrhea, often with blood or pus
- Abdominal pain or cramping, especially during bowel movements
- Unintended weight loss
- Fatigue, fever, and anemia
These symptoms are similar to those of other gastrointestinal disorders, underscoring the importance of seeking a proper diagnosis. A gastroenterologist can confirm the presence of ulcerative colitis through tests like colonoscopy and blood tests.
Ulcerative Colitis Symptoms and Causes
Ulcerative colitis is often characterized by its symptomatic flare-ups, which can vary in intensity and duration. One of the primary symptoms is persistent diarrhea often accompanied by blood or pus. Other symptoms can include abdominal pain and cramping, which is generally more severe during bowel movements. Unintended weight loss is also commonly observed, often resulting from loss of appetite or the body’s inability to absorb nutrients effectively. In some cases, individuals may experience fatigue, fever, or anemia.
Causes of Ulcerative Colitis
The exact cause of ulcerative colitis remains a subject of research. However, it is believed that genetic factors and environmental elements contribute to the development of the disease.
- Genetic predisposition: Research suggests that a family history of ulcerative colitis may increase the likelihood of developing the condition.
- Environmental triggers: These can include diet (such as a high-fat or low-fiber diet), stress, and exposure to bacteria or viruses.
- Overactive immune system response: In individuals with ulcerative colitis, the immune system mistakenly attacks healthy cells in the colon, leading to inflammation and ulcers.
Though ulcerative colitis cannot be cured, understanding its causes helps prevent flare-ups and manage the disease effectively.

Don’t Wait for Your Symptoms to Take Over. Start Managing Your Digestive Health Now!
Recognizing the signs early can make all the difference. If you’re dealing with symptoms of ulcerative colitis, we’re here to help you every step of the way:
- Fast, Clear Diagnosis: Skip the wait and get the answers you need with quick access to specialized tests.
- Personalized Treatment Plans: From medication to lifestyle tips, we’ll work with you to create a plan that fits your unique needs.
Difference between Crohn’s Disease and Ulcerative Colitis
While both are types of Inflammatory Bowel Disease (IBD), Crohn’s disease can affect any part of the gastrointestinal tract, whereas ulcerative colitis specifically targets the colon and rectum. Additionally, Crohn’s disease often causes deeper inflammation, while ulcerative colitis is limited to the lining of the colon.
| Feature | Crohn’s Disease | Ulcerative Colitis |
| Affected Area | Can affect any part of the GI tract | Only affects the colon and rectum |
| Depth of Inflammation | Affects deeper layers of the bowel wall | Inflammation is limited to the mucosal lining |
| Symptoms | Abdominal pain, diarrhea, weight loss, fatigue | Diarrhea, blood in stool, abdominal cramps |
| Location of Disease | Can occur anywhere along the digestive tract | Restricted to the colon and rectum |
| Treatment Options | Biologics, corticosteroids, and surgery | Medications, biologics, and surgery in severe cases |
How Is Ulcerative Colitis Diagnosed?
You must visit the best doctor for ulcerative colitis near you to get your condition diagnosed in detail. The diagnosis includes several tests, including:
- Colonoscopy: A procedure to view the lining of the colon and confirm the presence of ulcers or inflammation.
- Blood tests: To check for anemia or signs of inflammation.
- Imaging tests: To assess the extent of inflammation or complications.
Diagnosis is important to differentiate ulcerative colitis from other gastrointestinal disorders, such as Crohn’s disease.
How to Treat Ulcerative Colitis Naturally
Ulcerative colitis treatment options vary depending on the severity of the disease. The primary goal of treatment is to reduce inflammation and maintain remission. Both medication and lifestyle changes play crucial roles.
- Medication: Corticosteroids, immunosuppressants, and biologics are commonly prescribed to reduce inflammation.
- Surgical intervention: In severe cases, surgery may be necessary to remove the colon.
Natural treatment options, such as a diet plan for ulcerative colitis patients rich in fiber and anti-inflammatory foods, may complement medical treatments and help manage symptoms.
Best Treatment for Ulcerative Colitis 2026
As of 2026, new biologic treatments, including anti-TNF therapies and other biologics, are becoming available and provide promising results for many patients. These treatments are more targeted and effective in reducing inflammation in the colon.
Here are some of the best options available:
- Anti-TNF therapies (e.g., infliximab, adalimumab) – Target and block the inflammatory proteins causing damage in the colon.
- Biologics (e.g., vedolizumab, ustekinumab) – More targeted treatments that help reduce inflammation and promote healing.
- Corticosteroids (e.g., prednisone) – Reduce inflammation during flare-ups and maintain remission.
- Surgery – May involve the removal of the colon for severe cases where other treatments are ineffective.
For individuals with mild to moderate cases, biologics and corticosteroids may be the best treatment for ulcerative colitis. For those with severe cases, surgery may provide the most effective relief.
How to Manage Ulcerative Colitis Flare-ups
Managing ulcerative colitis flare-ups requires both medical intervention and lifestyle adjustments.
- Medication: Prescribed drugs, including biologics and immunosuppressants, can help manage flare-ups.
- Diet: Avoiding trigger foods and following a personalized diet plan for ulcerative colitis can reduce flare-up frequency.
- Stress management: Since stress can exacerbate symptoms, stress-reduction techniques like yoga and meditation are encouraged.
How Do You Prevent Ulcerative Colitis?
Although ulcerative colitis cannot be fully prevented, certain lifestyle changes can reduce the risk or delay its onset. Managing stress, maintaining a healthy diet, and avoiding triggers can help prevent relapse.
- Healthy, balanced diet: Rich in fiber, fruits, and vegetables.
- Manage stress: Practice stress-reduction techniques like yoga or meditation.
- Regular exercise: Helps improve overall health.
- Avoid smoking: Smoking may worsen symptoms.
What Foods Trigger Ulcerative Colitis?
Certain foods can trigger symptoms or flare-ups of ulcerative colitis. Identifying these triggers and avoiding them can help manage the condition effectively.
- Dairy products: Can cause discomfort in some patients.
- Spicy foods: May irritate the digestive system.
- Caffeinated beverages: Can exacerbate symptoms.
- Alcohol: Can inflame the digestive tract.
- High-fat or fried foods: May irritate the colon.
Diet Plan for Ulcerative Colitis Patients
A carefully curated diet plan for ulcerative colitis can help manage symptoms and improve overall health. A balanced diet rich in fiber and lean proteins, and low in processed foods, is highly recommended. However, some foods may trigger flare-ups. Keeping a food diary can help you identify personal triggers, allowing you to make informed dietary choices.
Diet Tips for Ulcerative Colitis Patients:
- Fiber-rich foods like fruits, vegetables, and whole grains help improve digestion.
- Lean proteins such as chicken, turkey, and tofu can be included.
- Avoid dairy products, which may cause discomfort in some patients.
- Spicy foods can irritate the digestive system and should be limited.
- Caffeine can exacerbate symptoms and should be reduced or eliminated.
- Processed foods should be avoided, as they may worsen inflammation.
Can Ulcerative Colitis Be Cured?
While ulcerative colitis cannot be cured, it can be effectively managed with medication and lifestyle changes. Early detection and treatment are critical for maintaining prolonged remission.
Living with Ulcerative Colitis: Managing Symptoms and Enhancing Quality of Life
Living with ulcerative colitis can be challenging, but with the right gastroenterology tests and procedures, and certain lifestyle changes, individuals can lead normal lives. It is crucial to prioritize self-care, adhere to treatment plans, and make necessary lifestyle adjustments.
Being aware of ulcerative colitis treatment options and how to treat ulcerative colitis naturally can significantly improve a patient’s quality of life and reduce flare-ups.
For personalized treatment, it’s important to contact a board-certified gastroenterologist near you. For more information or to schedule a colonoscopy, contact Gastroenterology Associates of Tidewater at (757) 547-0798.
Frequently Asked Questions
How does ulcerative colitis affect pregnancy and fertility?
Most women with ulcerative colitis can have healthy pregnancies. However, planning is key; achieving remission before conception and consulting your doctor about medication safety ensures the best outcomes for both mother and baby.
What is the difference between a “low-residue” and a “low-FODMAP” diet?
A low-residue diet limits high-fiber foods to rest the bowel during flares. In contrast, a low-FODMAP diet reduces specific fermentable carbohydrates that cause gas and bloating, helping manage overlapping IBS symptoms.
Are people with ulcerative colitis at a higher risk for colon cancer?
Chronic inflammation increases the long-term risk of colon cancer. Patients typically require more frequent colonoscopies, often every 1 to 2 years, starting 8 years after diagnosis to ensure early detection and effective preventive monitoring.
Can stress or smoking actually cause an ulcerative colitis flare-up?
While stress and smoking don’t cause the disease, they are significant triggers. Stress can aggravate the immune system, while smoking cessation, though vital for general health, can ironically sometimes trigger UC symptoms temporarily.