Managing ulcerative colitis (UC) requires an ongoing partnership with your gastroenterologist to ensure your condition is effectively controlled. UC, a chronic autoimmune disorder, affects an estimated 600,000 to 900,000 Americans, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Regular appointments with a GI doctor in Chesapeake, VA, are crucial to monitor your condition, discuss treatment options, and address any concerns that arise. With the right information and proactive management, you can better cope with the disease and lead a higher quality of life.
The more you understand your UC, the easier it will be to manage, ensuring that you’re always on the right path toward better health.

Table of Contents
What Should I Ask My GI Doctor About Ulcerative Colitis?
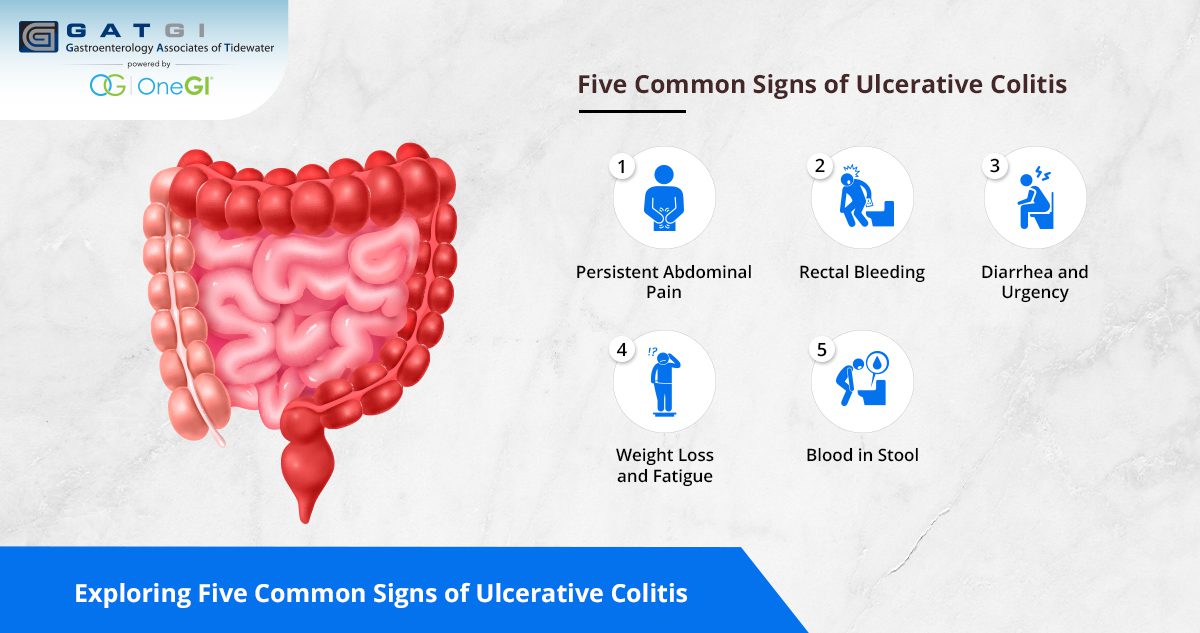
The first step after a UC diagnosis is to get a clear understanding of the type, location, and severity of your condition. These questions help define your treatment path and set expectations for symptom management and remission.
What Type and Severity of UC Do I Have?
Understanding the extent and type of Ulcerative Colitis (UC) is essential for creating an effective treatment plan. There are different types of UC based on the location and severity of inflammation in your colon. Knowing whether you have proctitis, left-sided colitis, or pancolitis is key to deciding your medication regimen. Ask your GI about these specifics during your appointment.
How Will My UC Be Monitored and Treated?
Knowing how your disease will be monitored helps you stay on top of symptoms. UC treatments range from aminosalicylates to biologics and steroids, depending on disease severity. Ask your ulcerative colitis gastroenterologist about potential treatment options, what side effects to expect, and how often you’ll need follow-up appointments and colonoscopies. This information is crucial for long-term disease management and determining how well your treatment plan is working.
What Should You Ask Your GI Doctor About Treatment Plans and Medication?
The right medication and treatment plan are pivotal in managing UC symptoms and maintaining remission. Asking about options, side effects, and effectiveness ensures you get a personalized approach that aligns with your needs and lifestyle.
What Are My Treatment Options for Ulcerative Colitis?
When discussing your treatment options, ask about the types of medications available to you, such as aminosalicylates for mild cases or biologics for moderate to severe UC. It’s essential to understand which medications your GI doctor recommends and why. Understanding whether your doctor is prescribing steroids for flare control or biologics for long-term remission can help you better prepare for the road ahead.
What Are the Side Effects of My Medication?
Knowing the potential side effects of any is crucial in managing your expectations. Ask your doctor about the risks associated with the medications they’re prescribing. This includes common side effects like nausea, fatigue, or changes in bowel movements, and more serious risks like infections or liver damage. Monitoring these side effects can help you manage any adverse reactions early.
How Will We Know if the Treatment Is Working?
Track progress together with your doctor. Ask what symptoms will improve first and how remission will be monitored. Your doctor may suggest regular lab tests, colonoscopies, or stool markers to track disease activity and inflammation. It’s important to understand how your doctor will measure progress so you can be prepared for follow-up visits and potential adjustments to your treatment plan.
What Lifestyle Adjustments Should I Make to Manage UC?
Lifestyle changes, including diet and stress management, play a significant role in controlling UC symptoms. It is one of the important doctor visit questions for UC patients. Your doctor can guide you on making adjustments that complement your treatment plan and help you manage your condition more effectively.
Should I Change My Diet Due to Ulcerative Colitis?
While no single diet cures UC, certain foods can exacerbate symptoms during a flare. Your GI doctor can guide you on what foods to avoid during flares, like gassy foods such as broccoli or whole grains. Ask about diet modifications during flare-ups versus remission. Additionally, a dietitian referral may be helpful to ensure balanced nutrition and a diet that supports your long-term health.
Should I Keep a Food and Symptom Diary?
A food and symptom diary can help you track what triggers UC flare-ups. Ask your doctor if maintaining a diary of food and ulcerative colitis symptoms is advisable. Many people find that tracking their meals helps identify specific foods that worsen symptoms. Your doctor can help you interpret this data to adjust your diet and keep symptoms under control.
How Will UC Affect My Work, Travel, and Exercise?
UC symptoms can vary, so it’s helpful to know what adjustments might be needed in daily life. Ask your doctor about exercise limitations, travel tips, and how UC will impact your energy levels. Knowing when you need rest or hydration can help you better navigate day-to-day activities without triggering flare-ups.
What Are the Long-Term Monitoring and Complications of UC?
Long-term management of UC involves monitoring for complications and ensuring effective treatments. Regular screenings, colonoscopies, and lab tests help you and your doctor stay ahead of the disease and prevent serious health issues.
How Often Will I Need Follow-up Appointments and Colonoscopies?
Since UC is a long-term condition, regular follow-up appointments and colonoscopies are vital for monitoring your disease. Ask your doctor how frequently these check-ups will occur. Depending on your disease severity, you may need more frequent colonoscopies to monitor for complications like colorectal cancer. Your doctor will recommend the right timing based on your individual case.
What Are the Long-Term Risks and Complications of UC?
UC carries risks, especially if left untreated or poorly managed. Some potential complications include colon cancer, severe infections, and nutritional deficiencies. Ask your doctor about specific risks related to your condition and how they will monitor for complications over time.
Is Surgery an Option If Medications Fail?
If medications do not effectively control symptoms, surgery may be an option. Surgery, like colectomy, is considered when UC becomes refractory to medication. This could involve removing parts of the colon. It’s helpful to ask your doctor when surgery is considered and what that would mean for your quality of life.
How Can I Manage UC Flare-ups and Prevent Complications?
A clear plan for managing flare-ups is essential to avoiding unnecessary distress. Knowing when to seek urgent care or take action can help you prevent worsening symptoms and complications. So, here are immediate questions to ask your GI doctor after a UC diagnosis.
What Should I Do if I Experience a Flare-up?
Ask your doctor to explain the first steps if symptoms worsen, such as increased blood, pain, or urgency. Understand what medications or interventions you can use at home and when to reach out to your doctor for more immediate help.
When Should I Seek Urgent Care for a UC Flare?
It’s crucial to know when a flare crosses the line into something more urgent. Ask your doctor to outline specific symptoms that would require immediate medical attention, such as severe bleeding, dehydration, or fever. A clear action plan can reduce panic when things go wrong.
What Should I Know About Family Planning with UC?
If you’re considering starting a family, UC management plays a key role in your health. Discuss medication safety and genetic considerations with your doctor to understand the implications for both you and your future children.
Is My UC Controlled Enough for Pregnancy?
Ask your GI doctor if your disease is under control and what steps you should take before trying to get pregnant. Some medications for UC are safe during pregnancy, but others may need to be adjusted or stopped. Discuss your family planning timeline and make a plan.
What Is the Risk of My Children Developing IBD?
UC has a genetic component. Ask about the likelihood of your children developing UC and how you can monitor them early if needed. While the risk is higher than in the general population, the majority of children do not develop UC.
Key Takeaways
- Ask about the type, location, and severity of your UC to understand your treatment options.
- Clarify the treatment plan, potential medications, side effects, and how to monitor progress.
- Diet doesn’t cause UC, but knowing what foods to avoid during flares is essential.
- Long-term care includes monitoring for complications, frequent colonoscopies, and managing medication side effects.
- Always have a flare plan and know when to seek urgent care.
Managing and Treating UC Made Easy at GATGI! Book an Appointment Today!
Understanding Ulcerative Colitis doesn’t have to be overwhelming. By asking these key questions during your GI visits, you gain clarity on your diagnosis, treatment, and long-term management. Knowledge is power and to begin, visit GATGI today.
Ensure you’re fully informed, track your progress, and work closely with your GI to prevent flares and complications. With the right care plan, you can manage UC effectively and live well. So, schedule a gastroenterology in Chesapeake, VA and to learn more click here.
FAQs
-
What should I bring to my first appointment with a GI doctor after a UC diagnosis?
Here’s your Ulcerative Colitis first appointment checklist:
- Symptom log: Track frequency, urgency, blood, pain, fatigue
- Test results: Bring any relevant lab reports, stool tests, imaging, or colonoscopy notes
- Current medications: Include all prescriptions, over-the-counter drugs, and supplements
- Family history: Note any relatives with IBD or autoimmune diseases
- Questions: Write down any concerns or inquiries for your doctor
-
Can diet help manage UC symptoms?
While diet doesn’t cause UC, some foods can exacerbate symptoms during flares. Ask your doctor for personalized dietary advice and whether a food-and-symptom diary is beneficial.
-
How can I prevent UC complications?
Regular follow-ups, colonoscopies, and managing inflammation with the right treatment can prevent long-term complications like colon cancer and severe infections.
-
When should I seek urgent care for UC symptoms?
Seek urgent care if you experience severe bleeding, dehydration, fever, or significant worsening of symptoms. Having a flare action plan in place can help you act quickly when needed.
Are you looking for a trusted UC center near you in Virginia? Consider GATGI, a renowned center offering comprehensive UC treatment and care. Schedule an appointment with GATGI today to discuss your diagnosis, explore treatment options, and develop a personalized flare management plan.